In a recent study published within the International Journal of Infectious Diseases, researchers described two cases of human monkeypox (MPX) and deep skin infection.
Study: Monkeypox infection and bacterial cellulitis: a complication to search for. Image Credit: DonyaHHI/Shutterstock
Background
Human MPX is a zoonotic disease brought on by the MPX virus. MPX is endemic to some African countries, with just a few outbreaks outside the continent before 2022. MPX is characterised by rash, fever, and lymphadenopathy. Most patients present with moderate symptoms not requiring antiviral treatment or hospitalization. Nevertheless, some commonly described complications are encephalitis, pneumonitis, keratitis, deep tissue MPX abscess, and secondary bacterial infections.
The World Health Organization has declared MPX a public health emergency of international concern, given the high variety of cases since May 2022. There have been 588 MPX cases in Portugal until July 25, 2022, with a suspected sexual transmission mode. The current study described cellulitis as a complication of MPX in two patients.
Findings
One patient aged 34 was a male with Fitzpatrick phototype III skin. Previously, the patient was diagnosed with human immunodeficiency virus (HIV) infection and sort 1 diabetes mellitus. The topic had no history of international travel up to now three months. The patient complained of painful skin lesions, sore throat, and fatigue. The topic reported having 18 unprotected casual sexual contacts with men up to now 30 days.
On statement, an umbilicated papule was present in the suprapubic region. There have been no other oral/skin lesions on the time. The investigators also observed inguinal centimetric lymphadenopathy. Swab samples were collected from the oropharynx and genitalia. The topic tested negative for hepatitis A, B, and C, syphilis, herpes simplex virus 1/2 infection, and Neisseria/Chlamydia infection.
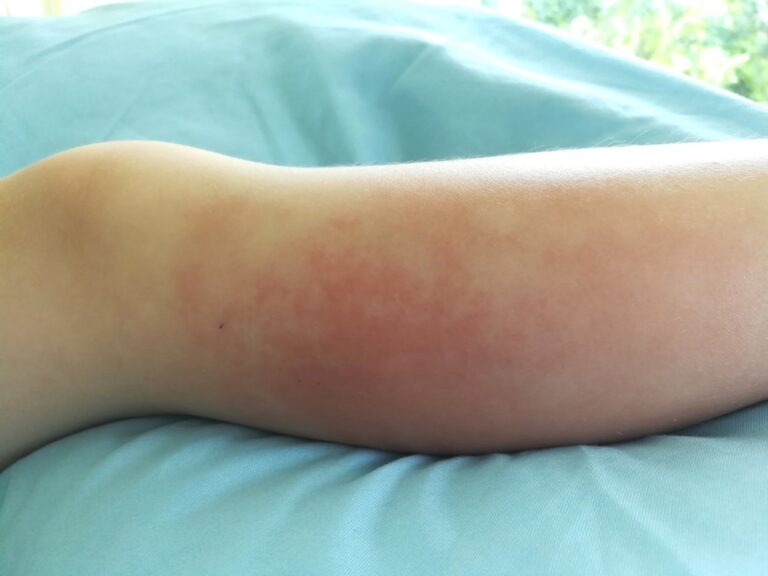
Eleven days after disease onset, the patient was hospitalized with edema, inguinal erythema, and native pain at the positioning of lymphadenopathy, compatible with inguinal and pubic cellulitis. Laboratory investigations revealed elevated C-reactive protein (CRP) levels without changes in lymphocyte count. The patient was began on oral flucloxacillin with clinical symptoms and cellulitis resolving after six days.
The second patient was a 35-year-old male with Fitzpatrick phototype IV skin. Previous medical history included antiretroviral treatment for HIV. The patient had no travel history up to now three months. The topic had three sexual contacts with men up to now 30 days. The patient presented with fatigue, skin lesions, and headache. Upon examination, there have been disseminated papules and pustules on the face, trunk, perianal and genital areas.
Six days after symptom onset, the patient was hospitalized for statement with edema, penile erythema, and pain compatible with cellulitis. Similarly, the patient had no changes in lymphocyte count but exhibited increased CRP. Clinical improvement with the resolution of cellulitis was observed seven days after treatment with oral flucloxacillin.
Conclusions
Treatment for MPX is really helpful during severe disease, for at-risk patients, and people with multiple complications. Since the two patients had less severe disease presentation, the team opted for a conservative approach to observe disease progression. Although deep skin infections are unusual during MPX, the progression of skin lesions with ulceration could generate entry portals for bacteria.
The authors posit that skin infections brought on by bacteria are under-reported in MPX patients, which could result in increased morbidity. Based on the empirical evidence, they suggested using topical antibiotics for ulcerations in patients with genital/perianal lesions and people with an increased risk of skin infections.